Young Investigator Award
Topic: 3. Heart Failure and Cardiomyopathy
Background
Once ICD has been implanted, device therapies worsen prognosis.
Hypothesis
CRT-D may reduce number of first appropriate ICD therapy, and independent factors can be identified.
Methods
175 consecutive patients (age 64.6±10.4 years, 23 [13.1 %] women), left ventricular ejection fraction (LVEF) 27.9 ± 7.6 % (range 10-50 %), 97 of ischemic origin, were treated, according to standard indications, with an ICD (in 80 cases the device was CRT-D) and followed-up during 2.5±1.5 years. Devices were placed for either primary (n=95) or secondary prevention (n=80).
Results
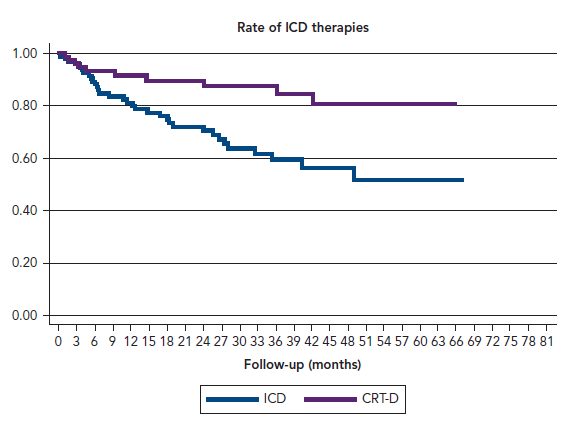
44 (25.1 %) patients received at least one appropriate therapy, 11.55 (8.57-15.57) per 100 patient-years. In the multivariable analysis, indication for secondary prevention was associated with a higher risk of first appropriate therapy (HR 3.42 [1.36-8.57] p=0.009), and CRT-D was associated to a lower risk of first therapy (0.31 [0.11-0.88] p=0.027). This reduction was present across all subgroups, even in patients in primary prevention (p=0.05), and although patients treated with CRT-D had significant lower ejection fraction and poorer NYHA class that their counterparts. In the follow-up, LVEF in patients with CRT-D improved from 25.3 % (5.6) to 37.0 % (5.6) (p=0.001). There were no differences in mortality in patients with and without CRT.
Conclusion
Although patients receiving CRT-D have a worse clinical profile, they receive less device therapies in comparison to those receiving an ICD; this reduction is associated with significant improvement in LV function.